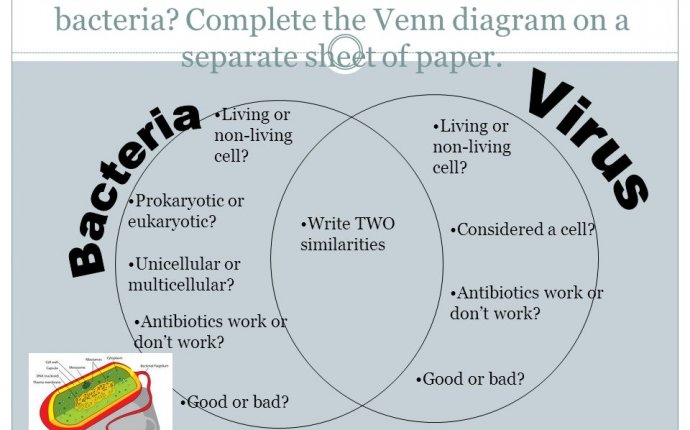
Bacteria and Viruses Similarity
The theory of molecular mimicry suggests that common pathogens, mostly viruses and bacteria, touch off autoimmune diseases when a person's immune system commits a colossal blunder, confusing foreign proteins with the body's own proteins. When immune system agents attack the pathogen, they also attack the body they are intended to protect.
Pathogens like bacteria and viruses have been implicated in autoimmune disease for some time, said Dr. Lawrence Steinman, a professor of neurology at Stanford University in Palo Alto, Calif. But convincing proof was lacking. New findings reported in the last two or three years, however, are offering more support for the idea in revealing biochemical mechanisms that may be involved.
Proponents of molecular mimicry still do not have definitive proof for their ideas, said Dr. Hugh McDevitt, an immunologist at Stanford. ''But I'd say the idea is more acceptable than ever, '' he said. ''It looks more and more feasible. But we haven't seen the final proof.''
Dr. Phillipa Marrack, an immunologist at the University of Colorado Health Sciences Center in Denver, said: ''They've found a smoking gun but they still don't know if the gun was pointing at the person who got sick. Maybe I'm asking too much, but they have to show me better proof.''
To understand how molecular mimicry is believed to work, consider two people who are exposed to the common coxsackie virus. When the virus enters the body of the first, it homes in on certain structures in her respiratory tract. Once inside those cells, it sets off an immune response. Her body wants to get rid of it.
The details of how this occurs are now well known. The virus is taken up by special cells that literally engulf it and chop the virus up into thousands of fragments. Each fragment is composed of 10 to 15 amino acids, which are the building blocks of proteins strung together like pearls in a necklace. A few of those fragments are then carried out to the surface of the immune cell (a macrophage, a dendritic cell or a B cell), and placed in a cleft or strategic pocket. The fragments literally dangle in the cleft, telling the body, ''Hey, I'm a foreign protein from the coxsackie virus. Come and get me.''
What gets to the cleft depends on the person's genes. She chops the virus into many different fragments but her genes determine which ones she will transport to the cleft. In this case, she carries only those fragments containing amino acids 15 through 30 of the coxsackie virus out to the cell surface.
The next step is also well understood. The body contains millions of circulating T cells, each of which is looking for a specific target - a protein fragment. Each T cell has a slightly different shape so every size and shape of protein fragment can be recognized.
Once a T cell docks onto coxsackie fragment 15 to 30, the T cell releases a flood of signals that initiate destruction of any tissues containing the virus. The immune system worked.
In the second case of exposure to the virus, the person's genes are different, so his immune system chops up the virus into different fragments. His so-called antigen presenting cells (the chop shops) send to the cleft fragments containing amino acid 80 through 95.
Here comes the blunder. It turns out that islet cells in his pancreas contain a protein, glutamic acid decarboxylase (GAD), that has the same amino acid sequence on its surface. The viral fragment mimics one of the proteins. But this person's immune system does not know this.
A T cell comes along, attaches to the fragment and begins to destroy all cells containing that fragment. Throat cells infected with the virus are killed. But the activated T cell and its troops go on a hunting expedition in the body, seeking any and all cells that show the fragment marker. When it finds such cells in the pancreas, healthy islet cells, the T cell is still bent on murder. It sets into motion a cascade of destruction. Islet cells die. The patient develops type 1 or juvenile diabetes.
For a long time, people did not think molecular mimicry was possible, said Dr. Eli Sercarz, a professor in the department of microbiology and molecular genetics at the University of California in Los Angeles. T cells that recognize proteins from their own body, so-called self proteins (like those on the second person's islet cells), were supposedly all killed off in the thymus early in life. The thymus, a kind of T-cell nursery, contains a master list of the body's most abundant proteins. When T cells are born, they are compared with the master list and those that match self-proteins are killed off. T cells that recognize foreign proteins are released into the general circulation. In this way, the body should not manufacture T cells that would destroy self-tissue.
But recent research shows a different picture, Dr. Sercarz said. Some proteins, including constituents of brain and the GAD protein in islet cells, are not on the thymus master list. So T cells that recognize these proteins are not destroyed. They enter the circulation. Other immune factors suppress these self-reactive T cells, he said, holding them under tight control. When that control is lost, an autoimmune disease can ensue.